Cervical osteochondrosis or osteochondrosis of the cervical spine is a common disease of knowledge workers. Disease with rapid progression. It is osteochondrosis of the cervix, complicated by the development of disc herniations, that is associated with an increased incidence of early strokes. For diagnosis, an MRI scan is required.
What is cervical osteochondrosis?
Osteochondrosis of the cervix is a common cause of neck pain, headache, increased pressure, shoulder pain, numbness in the fingers, pain under the shoulder. Currently, the frequency of cervical osteochondrosis has increased significantly as the role of the computer in our lives has increased.
However, a fall or injury can stimulate the onset of osteochondrosis and degeneration (forgetting) of the intervertebral discs over time can lead to symptoms.
Symptoms
In addition to moderate or mild pain, a feeling of stiffness in the neck, and, in some cases, impaired mobility, many patients with cervical osteochondrosis experience numbness, tingling, and even weakness in the neck, arm, or shoulder as a result ofchemicals. irritation and tight nerves in the cervical spine.
For example, grabbing a nerve root in the C6-C7 segment can cause weakness in the triceps, shoulder, or forearm muscles, weakness in the wrist muscles, causing the hand to "hang, " and a change in tenderness in the finger. secondary.
Osteochondrosis of the cervix also often leads to the development of spinal canal stenosis and other progressive conditions, such as intervertebral hernia. How does this happen?
Osteochondrosis is nothing but degeneration of the vertebral structures, caused, as a rule, by the natural aging of the body. With age, ligament thickening, the formation of bone growths in the vertebrae, and other changes occur. When spinal ligaments thicken or bone growths appear, as well as for a variety of other reasons, there is less space for the spinal cord and nerves within the spinal canal. This condition is called stenosis, d. m. th. narrowing of the spinal canal. Severe narrowing of the spinal canal can lead to compression of the nerve roots or even to the spinal cord itself.
Intervertebral hernia is also, in most cases, a consequence of degeneration. Intervertebral discs serve as shock absorbers between the vertebrae, thus preventing their destruction. Over time, the disc loses moisture and nutrients, flattens, becomes more brittle and less elastic. As a result, a crack may form in the ring, through which a portion of the pulposus nucleus is squeezed into the spinal canal. This condition is called an intervertebral hernia. If an intervertebral hernia compresses a nerve root nearby, pain syndrome and / or related neurological symptoms occur.
Diagnosing
Successful diagnosis of cervical osteochondrosis begins with consulting a doctor. The doctor compiles the patient's medical history and performs a physical examination to check the mobility and sensitivity of the neck. During the examination, the patient may be asked to perform certain movements and report how the pain symptoms change (increase or decrease).
If the examination shows that further tests are needed, your doctor may recommend radiographic tests such as radiographs, magnetic resonance imaging (MRI) or computed tomography (CT) scans. These diagnostic examinations, with varying degrees of reliability, can confirm the presence and localization of osteochondrosis, as well as identify other conditions (for example, calcification or arthritis) that may be the cause of the patient's symptoms.
The best option for radiographic examination at the moment is MRI, because With the help of a magnetic resonance imaging, it is possible to obtain high-quality detailed images not only of bone tissue, as in radiography, but also of soft tissuespine, including muscles, ligaments, vessels, nerves, and intervertebral discs. CT is usually prescribed if there are any contraindications to MRI, the main of which is the presence of metal structures or equipment in the body (artificial joints, pacemakers, etc. ). The quality of CT scans is lower than that of MRI scans, but they can also show the condition of the soft tissues of the spine.
Treatment of cervical osteochondrosis
Conservative (non-surgical) treatment of osteochondrosis is always recommended as the main strategy and surgical intervention is considered only if complex conservative treatment for at least six months has not yielded results or if pain and other symptoms significantly interfere with the patient's daily activities. .
Methods used in the conservative treatment of cervical osteochondrosis may include:
- spinal traction (traction). Spinal cordless traction methods, which have been used recently, allow to completely eliminate the complications of this method of treatment, without which load traction can not do. With an increase in intervertebral distance, nutrition of all intervertebral discs improves, pain syndrome disappears.
- Corrective gymnastics. . Corrective gymnastics can improve spinal mobility. In the mobile vertebral segment, hernias and extensions do not grow or form as the intervertebral discs perform their function.
- masotherapy.
- drug therapy. Includes NSAIDs (non-steroidal anti-inflammatory drugs) and painkillers. In most cases, drug therapy has little or no temporary effect.
- cervical corsets, orthopedic pillows. They can be recommended to stabilize the cervical spine and reduce pressure on the nerve root after trauma and fractures of the spine.
Surgical treatment of cervical osteochondrosis
If there is no significant relief after six months of conservative treatment and the daily routine becomes difficult for the patient, surgery may be considered. Typically, for cervical osteochondrosis, a procedure called spinal fusion is performed to immobilize the affected vertebral segment. This surgery involves removing the intervertebral disc, decompressing the nerve root, and placing a bone or metal implant to maintain or create a normal disc space and stabilize the spinal segment.
As a rule, the fusion of the spine is performed in a vertebral segment; in rare cases, the issue of performing surgery on two vertebral segments may be considered. Either way, the patient should know that surgery to relieve the symptoms of neck pain is much less likely to lead to positive results than a similar surgery to relieve pain in the side with cervical osteochondrosis. Therefore, if neck pain is the main or only symptom, spinal fusion should be recommended only as a last resort or if all conservative treatments have been tried and failed. If disc space can not be identified as the most likely source of neck pain, it is best to avoid surgery, even if conservative treatment does not offer significant pain relief. Furthermore, do not forget that spinal surgery can be fraught with quite serious consequences both in the operated area (local infection, implant rejection, etc. ) and for the whole body (blood clots, allergic reactions to medications, etc. ). . Therefore, before making a decision on surgical treatment, it is necessary to discuss all the details of the operation directly with the surgeon who will perform it. It should also be noted that cervical spine surgery most often leads the patient to vertebral disability.
What is cervical osteochondrosis?
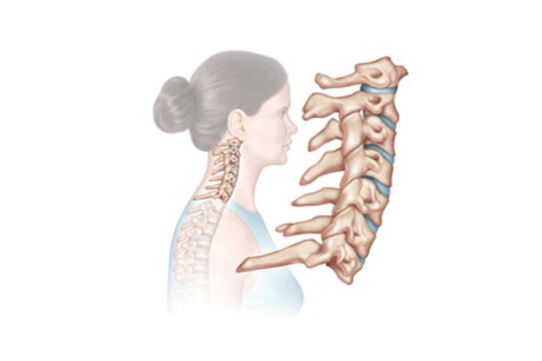
Formal medicine interprets osteochondrosis as a degenerative-dystrophic lesion of the intervertebral discs.
From which part of the spine these discs are located is also given the definition of the disease.
Let's specifically look at the symptoms of cervical osteochondrosis, which accounts for almost 80% of all spinal diseases.
The sad factor is that the disease affects the category of patients aged 30 to 50 years, ie at the peak of their ability to work.
In young people, the disease acts as an independent disease, at an older age it is already a pathology that has developed against the background of other diseases of the joints.
How does the disease develop?
For each part of the spine, a phased development of the disease is characteristic. Osteochondrosis of the cervix does not go beyond this framework, so it is worth dwelling on the details in each of its stages.
- In the initial stage, there is a gradual destruction of the intervertebral discs. Between them is an annulus fibrosus, in which cracks appear, leading to a decrease in the elasticity and strength of the discs themselves. They shrink and compress the nerve roots.
- The second stage is a consequence of the first untreated stage. The initial destruction of the discs flows into a chronic form, tissue compression occurs, dislocations of the cervical vertebrae are observed. Head drop syndrome often develops at this stage.
- In the third stage, the sensations of pain intensify, persistent headaches appear, the sensitivity of the upper limbs is lost and the "lumbago" of the cervix suffers. This is due to the fact that the fibrous ring at this stage is almost completely destroyed.
Often, there is a reduction in third-degree cervical osteochondrosis pain sensations. This occurs at the moment when the cartilage tissue disappears and there is nothing to hurt.

Causes
Given the prevalence of osteochondrosis in general, doctors began to study its causes closely. Many of the negative factors have been identified, but there is no definitive list. Here are the ones that have been announced to date:
- sedentary lifestyle;
- all kinds of intoxications and infections;
- great physical activity;
- smoking;
- continuous weight gain;
- stress and nervous tension;
- uncomfortable shoes or a messy foot that creates unnecessary pressure on the spine;
- improper nutrition;
- frequent hypothermia and exposure to bad weather;
- age-related changes;
- spinal cord injury;
- poor inheritance;
- a sharp refusal to train, if they have previously done them for a long time.
By getting acquainted with the reasons, it becomes clear that cervical osteochondrosis can occur at any age. And if at first the symptoms of osteochondrosis are insignificant and are characterized by infrequent attacks of pain, then over time it turns out that it is impossible to rotate even the neck, and it is difficult to tilt the head. And these are not the only risks of the disease.
What is the risk of the disease
Our neck is a great worker. She is involved throughout the day and her small beads stoically resist all the twists and turns of the head. If the bones are displaced, the nerves are compressed and the blood vessels are constricted, and the vertebral artery, which is responsible for nourishing the brain, also passes through the cervical spine. The artery is compressed, the nerve root is compressed and the inflammatory process begins.

What does this lead to? Spinal cord injury, ischemia, intervertebral hernia - these are the severe consequences of osteochondrosis of the cervix. Here we add a general decrease in mobility and osteophyte formation. As a result, we have a disability that threatens complete immobility. With such a disappointing prognosis, it is important to quickly recognize the symptoms of cervical osteochondrosis.
Symptoms

The shortest way to identify osteochondrosis is patient complaints. So how does a person feel if his or her cervical vertebrae are destroyed? The picture of the disease looks like this:
- dizziness;
- Severe headache;
- "Flies" and colored spots on the eyes on the background of headache;
- pain when turning, lifting weights;
- pain radiating to other organs (heart region, other organs).
Sometimes the signs of osteochondrosis can be listed among other diseases, but they can not be ignored, even if they are temporary.
Diagnosis and treatment
Following the sensations expressed by the patient, the neurologist moves on to a more accurate diagnosis of the disease. A few years ago, only X-rays were in the arsenal of doctors for the diagnosis of osteochondrosis. Computed tomography and magnetic resonance imaging are actively used today. They allow you to accurately determine the stage of the disease.
After evaluating the resulting figure, a vertebroneurologist specialist prescribes the necessary treatment. The first thing the doctor takes is to relieve the pain, then the swelling and inflammation. To relieve pain, such anti-inflammatory drugs are used. As we recall, the compression of the vertebral artery disrupts the supply to the brain, which means it needs to be improved. This is done with the help of muscle relaxants.

Knowing that the symptoms and treatment of cervical osteochondrosis are related to the spine, massage and physiotherapy exercises are necessarily included in the complex of measures to improve health. The massage is performed by a professional and by the patient himself. There are also special exercises aimed at developing the cervical vertebrae and restoring their mobility.



















